Office Surgical Procedures: Plantar Warts/ Verrucae
- June 17, 2019
-
Clayton Clews
- Uncategorized
Podiatric Medicine: Office Surgical Procedures and Local Anaesthesia Techniques
In this blog, I will discuss office surgical procedures and local anaesthesia techniques I commonly utilise in my private practice rooms. These surgical techniques usually permanently resolve the patient’s foot complaint. Local anaesthesia techniques, with and without cortisone, reduce/eliminate pain and can be used in addition to other types of treatment to maximise patient outcomes. Part Two of this blog will focus on the verrucae pedis (plantar wart) curettage procedure.
PART TWO: Verrucae Pedis (Plantar Warts) Curettage Procedure
Verrucae pedis lesions, more commonly known as ‘plantar warts’ are a common benign soft tissue lesion affecting the foot. They are common across all age groups, but probably affect children more so than adults. A plantar wart is a growth between the epidermis and dermis (the two top layers of skin) caused by a viral infection which penetrates and infects it. It is common to find plantar warts on the weight bearing surfaces of the feet, including the toes. Because they are subject to pressure and friction they will often become painful, particularly with increased periods of standing, walking and running activities. Plantar warts are usually surrounded by thickened skin (hyperkeratosis) and hence any treatment should include removal of as much of this as possible.
A curettage procedure involves an incision into the epidermal and dermal layers surrounding the verrucae (wart) lesion followed by the use of a curette (an instrument in the shape of handle with a small scoop at one or two ends). It is this scoop which undermines the encapsulated wart lesion and separates it at the level of the junction between the epidermis and the dermis. Phenol can then be used to chemically cauterise the surgical site, dealing with any residual remaining verrucae pedis cells.
This procedure is performed with the use of a local anaesthetic initially, to numb the surgical site, either through direct infiltration into a region or via an area block, such as a tibial nerve block. Further local anaesthetic, combined with adrenaline (usually used in a concentration of 1:100 000 or 1: 200 000) is infiltrated into the region of the foot where the plantar warts is positioned and is used to achieve haemostasis, or stop the surgical site from bleeding. This is very important, for without a relatively bloodless field, the procedure would be difficult to perform, the phenol would be neutralised by the blood and the surgery would be very messy! Safety of course is enhanced in a near bloodless field of work.
Figure 1 Figure 2
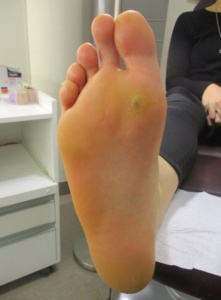
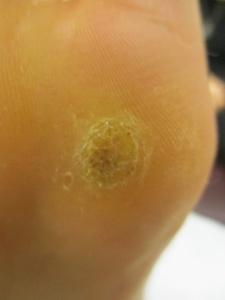
Figure 3
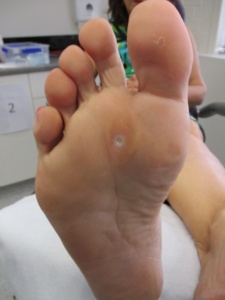
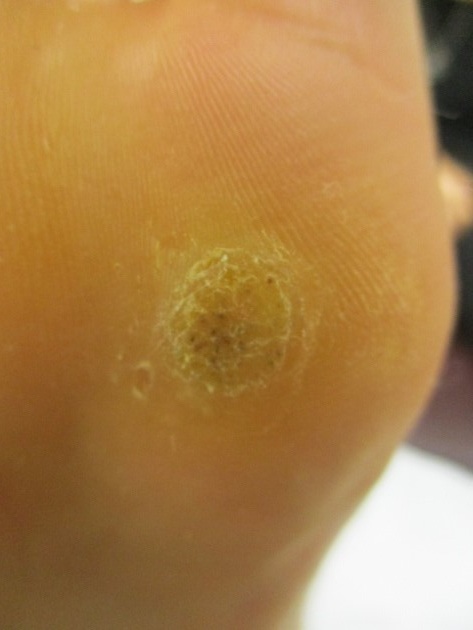
Figures 1 & 2: These pictures demonstrate a typical isolated plantar wart, which caused the patient considerable pain because of its size and location. Isolated plantar warts or small numbers of these respond very well to the curettage with cautery technique. Figure 3 demonstrates a porokeratosis, which is a type of fibrous corn and can be confused for a plantar wart. Such a lesion is common in smokers and will not respond to a curettage procedure.
Figure 4 Figure 5
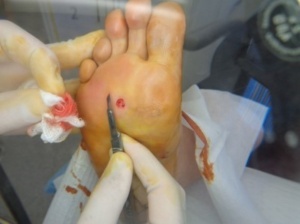
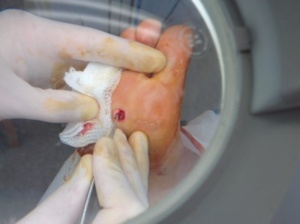
Figure 6
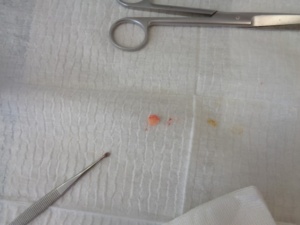
Figures 4-6 demonstrate the curettage and cautery procedure. After the plantar wart has been curetted (Figure 4) it is cauterised typically with liquified phenol. The removed lesion is often quite small (ie – 5mm x 5mm) and has the texture of rubber. A good compression dressing with plenty of post is highly advised after the procedure.
The verrucae pedis curettage (with cautery procedure) is highly reliable at definitively removing plantar warts, with minimal scar tissue formation. It is a terrific procedure as it eliminates the requirement of multiple consultations, commonly involved with cryotherapy and other non-surgical techniques. Patients’ simply get frustrated and tired of having to attend multiple times (not to mention the costs involved) for treatment, hoping that one day they may hear good news, in that their warts have finally gone! With the verrucae curettage technique, the warts are excised and permanently removed off ‘one’ consultation (with a further two post-operative review consultations). The rest of the time, they are simply healing from their procedure, which usually takes from 2-4 weeks.
An important component of the procedure is for the use of a highly padded compression dressing. This will provide the patient with consistent comfort immediately following the procedure and during the subsequent two or so weeks. A proper dressing will also incorporate antiseptic dressings greatly reducing the risk of infection, which is uncommon with this technique.
Suite 8 (Ground Floor), 146 Scollay St, Greenway ACT 2900
6287 4889
6293 2325
[email protected]
ACT Podiatry : Advanced Foot & Ankle Centre
Canberra Podiatric Surgeon
Suites 16-17 (First floor) 14-16 Brierly St, Weston ACT 2611
6287 2818
6293 2325
[email protected]
ACT Podiatry : Advanced Foot & Ankle Centre
Canberra Podiatric Surgeon
Copyright © 2018, ACT PODIATRY | SEO by High Jump Digital

