Footwear and Diabetes: What you need to know
- February 14, 2020
-
Romany Vonarx
- Recent Articles, Uncategorized

Footwear and diabetes – what’s right for me?
Living well with diabetes is easier when you have the right information. It can be hard to know what suits your situation because there is such variation in the experience of living with diabetes. When it comes to footwear, walking or exercise, there are some general guidelines to follow to get you stepping in the right direction.
As podiatrists, we’re encouraged to assess the risk of each individual with diabetes using standardised testing and report the risk levels as low, medium or high. When you have your annual diabetes assessment with your podiatrist at ACT Podiatry, they will discuss the results with you. The results of the assessment and risk classification will form the basis of your treatment plan. We will recommend individualised measures for you to take at home with the aim of preventing any foot problems associated with diabetes.
Low risk of developing diabetic complications
You have a diabetes diagnosis but your testing finds you have functioning protective sensation, good blood flow and no foot deformity. You can trust what your feet are telling you when you have protective sensation, so problems with footwear will usually present painfully. Things like a folded sock or developing blister are painful, so you stop and check your feet before too much damage is done. It is important that your footwear supports your lifestyle and any exercise you wish to participate in as well as protecting your feet from injury. Your shoes need to be task specific- work boots for gardening, hiking shoes for hiking, sandals for hot weather when there is no risk of injury. Your shoes need to be well fitted and accommodate any foot deformities you may have.
Moderate or high risk of developing diabetic complications
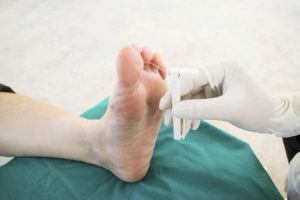
An annual foot check is recommended for people with diabetes
You have a diabetes diagnosis and your testing finds you have one, two or all three of: reduced nerve function, reduced blood supply, and foot deformity. Often you have had diabetes for 10 years or more. When there is a loss of protective sensation you can’t trust what your feet are telling you. Often early injury to the feet will go unnoticed and a severe injury can develop. When foot deformity is present, it increases the likelihood of high pressure areas where wounds or pressure sores and blisters can develop. This effectively increases the risk of injury to the feet. When there is reduced blood supply or poor blood quality, it can increase the expected healing time of any injuries that you do acquire. Combine longer healing time, with increased risk of injury from two factors, and your feet need careful attention to prevent injury in the first place. Footwear, in these cases, plays an integral role in protecting the feet from trauma and injury. You’re looking for footwear that fits well, has smooth linings and accommodates any deformities you might have. Footwear that has extra depth, accommodates custom orthoses and has adjustable fitting features can be really useful. Getting fitted properly and buying quality shoes that will last the distance is an important move in your foot health care.
What makes a ‘good’ shoe?

It is useful if footwear has removable insoles
When patients with diabetes ask what is a good shoe for them, our advice is that a ‘good shoe’ for a person with diabetes is a ‘good shoe’. But what does that mean to you?
As a general rule, ‘good’ shoes, as recommended by a podiatrist, will feature the following:
• A firm heel counter – can’t press it down with your thumb
• A firm mid sole from heel to mid foot – can’t significantly twist the shoe with hands around the heel and ball of foot area
• A removable innersole
• A bend only where your toes bend up when you press from heel to toes
• Laces or similarly flexible fastenings (like velcro)
Shoes like this provide flexibility in therapies; so we can fit offloading or orthoses into your shoes if we need to. They also last well and provide support and protection for your feet on a daily basis.
So, if you are at low risk of developing diabetic foot complications, get yourself good shoes. It’s best if these are fitted professionally, which can happen at shoe shops with well trained staff, like Happy Fit Footwear. A good pair if shoes can cost hundreds of dollars, but if it’s too small or too big or plain the wrong shape for your foot, then it may pose problems or be uncomfortable for you.
If you are at high risk of developing foot complications from diabetes then there are a few more features of footwear that can become important. It is highly recommended that you get all of your shoes professionally fitted if you are high risk and even getting that fit checked by your podiatrist can be helpful too.
• Extra depth shoes – usually have multiple innersoles that come out of the inside of the shoe to provide more depth to fit in offloading orthoses. These can also be useful for people who have “deep” feet or high arches as there is more internal volume available within the shoe.
• Rocker bottom shoes – can reduce pain and redistribute loading in the foot but are very specifically prescribed due to an increase in falls risks with some people. Rocker bottoms can be tricky to get used to, so please only seek these out under specific guidance of your podiatrist.
• Medical grade footwear such as the Dr Comfort range available at Happy Fit Footwear and should be considered if you are assessed as being at high risk of developing a diabetic foot problem.
Remember, foot complications are avoidable in people with diabetes. Arm yourself with the correct knowledge and strategies for preventing foot problems by visiting ACT Podiatry regularly. Always ensure your footwear fits properly and is suitable for the activities you intend using them for. Mobility and quality of life start with happy feet!

Healthy Feet Enhance Mobility and Quality of Life
Suite 8 (Ground Floor), 146 Scollay St, Greenway ACT 2900
6287 4889
6293 2325
[email protected]
ACT Podiatry : Advanced Foot & Ankle Centre
Canberra Podiatric Surgeon
Suites 16-17 (First floor) 14-16 Brierly St, Weston ACT 2611
6287 2818
6293 2325
[email protected]
ACT Podiatry : Advanced Foot & Ankle Centre
Canberra Podiatric Surgeon
Copyright © 2018, ACT PODIATRY | SEO by High Jump Digital

